MUAC Approach, enabling Timely Diagnosis of Severe Malnutrition
Malnutrition-deficiencies, excesses,or imbalances in a person’s intake of energy and nutrients- remains a challenge in Uganda with over 250, 000 children still suffering from severe acute malnutrition.
According to the United Nations International Children’s Emergency Fund (UNICEF), malnutrition threatens to destroy a generation of children in Uganda. More than one third of all young children amongst whom 2.4 million are stunted.
Insufficient food at the household level coupled with parents’ ignorance is one of the factors fueling the rising cases of malnutrition among children in Uganda.
The Ministry of Health report from the routine Health Management Information System indicates that the number of severe and acute malnutrition admissions nearly doubled between January 2020 and October 2021.
This is perhaps what compelled the Uganda health ministry to launch a program in December 2021 through the innovative approach where families and other caregivers are now being empowered to diagnose signs of malnutrition in their children using Family-Led Mid Upper Arm Circumference (MUAC) tapes, instead of entirely relying on community health workers.
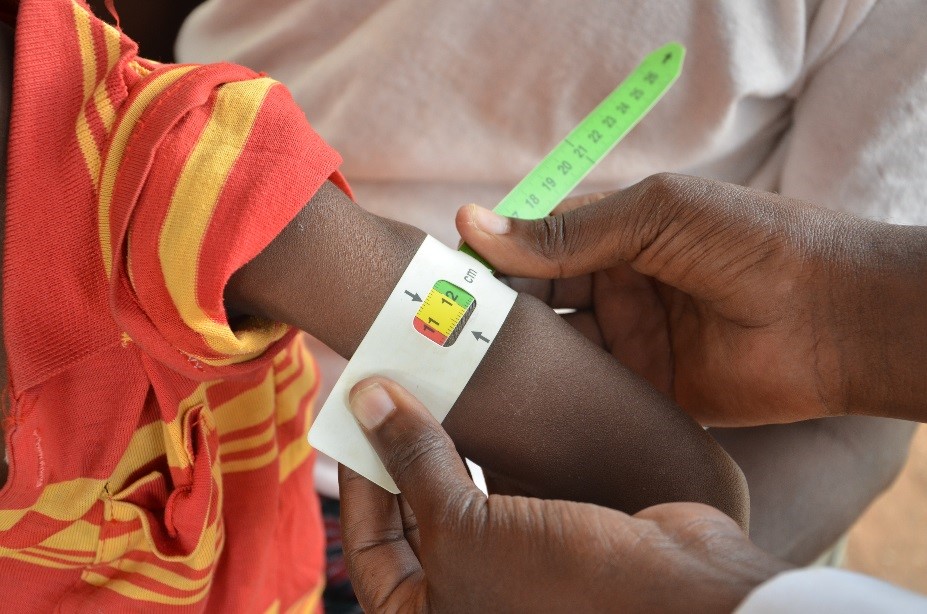
The MUAC tape, a long, colour-coded strip marked with graduated measurementshelps mothers and health workers quickly determine if a child is acutely malnourished. If the measurement of the girth of a child’s mid-upper arm is within the yellow part of the band, it indicates that the child is suffering from moderate acute malnutrition. If the measurement falls within the red part of the band, it indicates that the child is suffering from life threatening, severe acute malnutrition.
According to Zakaria Fusheni,a nutrition manager with UNICEF Uganda, it is estimated that only about one out of every ten children in Uganda consume a diet with the necessary food combinations for growth yet less than 20 per cent of children who require treatment for severe acute malnutrition were receiving it before the MUAC program was launched. He says the statistics are now gradually reflecting an upward trend of up to 40 per cent.
Zahara Nankungu who took her six-year-old son Ssenfuka Malik to Kimanya health center two in Masaka district for treatment says she received the MUAC band from a Village health team. “I was able to realize that my child needed professional help when I used the MUAC band that I placed on his mid upper arm and it went all the way in to the red area which I was taught is dangerous and life threatening,”she narrates.
“My Malik is now back on track, he is back to playing with the energy of a bull, running around all day and giving me a reason to be up on my feet all day. He’s is back to his happy normal self, thank God and thanks to the MUAC team.”
Nankungu says she is now a volunteer training other mothers on how to use the tape or when to seek professional help, she says they can now keep track on their children however the challenge comes in when they sometimes fail to find the right foods to feed their children as the food they can afford is not always as nutritious as what nutritionists recommend.
Also, she notes that most of her peers still attribute malnutrition to witchcraft, thus there is need for more sensitization.
Mugambe Jasper, a three-year-old, has been suffering from malnutrition.Together with his mother, they have been admitted at the Mulago National referral hospital, nutrition ward commonly known as the Mwanamugimu ward where they were referred from Kasese District. He has been enrolled on therapeutic foods treatment.
The Manamugimu Nutrition ward is Located on the northern side of Mulago National Referral Hospital. It is Uganda’s prime centre that medically handles nutrition complications in children.
The ward has over 60 health workers who include doctors, clinical officers, nurses and administrative assistants dealing with urgent cases that cannot be handled by other facilities that do not primarily focus on nutrition.
Through UNICEF support, children like Malik and Mugambe suffering from severe acute malnutrition are able to receive lifesaving ready-to-use-therapeutic foods also known as RUTF, an energy-dense food that is enriched with micronutrients.
Complications resulting from malnutrition are currently widespread in Uganda, affecting about 54% of children, about 15 million of the country’s 25 million children. The incidence is even higher among the under five-year-olds, with one out of three children stunted.
Mugambe is currently taking treatment at the ward under close monitoring as well as therapeutic foods provided free of charge at the ward. His mother is now being taught how to prepare these foods and how to manage him once they are discharged and sent back to Kasese.
She will also leave with disposable color-coded MUAC tapes which are currently being distributed to mothers at health center IIs to enable detect signs of malnutrition, provide appropriate care and seek treatment at health facilities early enough. They are first shown how to use them and subsequently carry out routine checks through the MUAC.
Mugambe’s mother Jenniffer Nyakabaale is however worried that her child might regress once she goes to Kasese because she cannot afford the foods offered at the ward being that the market where she was vending food was closed during the outbreak of COVID-19.
“We aim to give a holistic treatment, so beyond feeding the children and teaching their caretakers how to properly feed them, we want to help ward off the trauma caused by their sickness. We have a facility where they go to play, relax and learn,” says Julie Wamala, a nutritionist at Mwanamugimu ward.
She adds that they have now realized that poverty is the major driver of malnutrition amongst children thus the need to now empower mothers and caretakers with information and skills on how to undertake and succeed at income-generating activities so that when they return home, they can have not only food but nutrient rich foods to feed their children.
Wamala explains that the first phase when a child is brought at the unit in a dire condition involves admitting the child to the resuscitation ward, also known as the Critical Care Unit where the child goes through the urgently-needed first steps to resuscitation.
Children here are treated for infections and fed on a special type of milk fortified with nutrients and drugs to revive their digestive and general body systems while some are even put on oxygen. Children at this section also called the Giraffe ward are normally very thin and most of them stay here for about three weeks before they improve. However, some improve faster, while others take as long as six weeks.
Now, Mugambe along with other children whose caretakers were able to diagnose them and later sought for help at the Mwanamugimu ward and other health facilities across the country are already on their way to full recovery thanks to the professional help they have received along with the consistent regimen of ready-to-use-therapeutic foods.
Dr. Elizabeth Kiboneka, the head of the Mwanamugimu nutrition unit says they would like to extend services across the country but for now, their capacity cannot allow unless they get support. The unit is currently funded entirely under the Mulago budget, and the only other support is of therapeutic feeds given in kind by UNICEF.
Jetress Ithungu, the Kasese District LC V Vice-chairperson, says that more than 50% of the children in the district are stunted either physically or intellectually due to food insecurity and poor feeding behaviors. She argued that many parents are selling off their food to meet the rising cost of living.
The stunted growth of children stood at 32% when a baseline survey was done across the seven parishes in this area but with interventions, this trend has drastically reduced to 18% which I would still say needs to reduce further, Ithungu said.
Francine Abwoch, a teenage mother says she had no idea that her 2-year-old child was suffering from acute malnutrition and thus never sought for help until it was too late.
According to Abwoch, Apio was a healthy bouncy baby girl at birth with a score of nine out of ten but her health deteriorated as she grew older. “I did not have any money to buy for my baby milk or food consistently so I would feed her on what I could get my hands on, the baby also suffered from many infections, her immunity was low and she tremendously lost weight. We sometimes had one meal in a day. That’s all I could afford because her father left us and I had to struggle alone but I lost my baby,” she narrates.
For Abwoch who is now an internally displaced person in the slums of Kisenyi in Kampala, poor nutrition coupled with infections that were never properly diagnosed and treated led to her baby’s demise.
She now has a one year old baby.Abwoch says she has been empowered enough now to diagnose malnutrition with her son at the Kisenyi health center III where she also acquired a number of disposable MUAC tapes that she uses to monitor his growth.
Kisenyi health center III now has a capacity reach of over 1000 mothers in central Kampala especially in the slum areas of Katwe, Kisenyi, Kikoni, Kasubi and Bwaise.
Despite this, most Ugandan health facilities lack a nutrition unit which is vital for the rehabilitation of severely malnourished cases. Inadequate nutritionists across all districts, also remains a challenge. As a result, some organizations are also using other interventions.
Esther Wamono, a Nutrition Surveillance Officer with Action Against Hunger in the Karamoja region of northeastern Uganda says some of the common nutritional problems in the Karamoja communities are fueled by poor hygiene and sanitation conditions.
People who don’t have access to latrines, hand-washing stations, and safe drinking water and other basic sanitation are much more likely to contract cholera, dysentery, diarrhea, hepatitis E, and other diseases that can also lead to malnutrition.
“We’re addressing this problem in a variety of ways: we’re working with families to improve sanitation and hygiene in their homes, we’re helping them construct and maintain household latrines, and we’re digging bore holes to ensure they can access clean drinking water. People don’t always realize how important clean water is in combating malnutrition, but it’s critical,” she adds.
“Tackling malnutrition requires collective effort, right from the family level and in a timely manner,” Fusheini says, adding whereas prevention and treatment of severe acute malnutrition among children cannot be postponed, the COVID-19 pandemic continues to restrict the number of children who can be reached with these life-saving services.
According to Fusheini, there are still thousands of Ugandan children at the verge of losing their lives to severe acute malnutrition due to government’s restrictions to control the spread of COVID-19 and the two countrywide lockdowns that disrupted the production, transport, and sale of nutritious and affordable foods, pushing millions of families towards nutrient-poor alternatives.
Dr. Olaro Charles another expert cites the need for mindset change saying malnutrition is a national problem that needs urgent attention. He says good nutrition is a preventative measure for diseases. It is like a vaccine for good health.
Dr. Aggrey Batesaki on the other hand says what is crucial is raising awareness on the simplified evidence-based and practical solutions on nutrition for mothers and children. “Early detection and referral of children with malnutrition is important for treatment,” he stresses.
Dr. Batesaki’s concern however, is that whereas the village health teams are supposed to reach out to children to detect and refer those malnourished to health facilities, they are usually overwhelmed with other competing priorities and thus many children lie unidentified in the community due to limited screening and some do even die before reaching health facilities.
This story was first published in Metro fm 90.8
